Note: This article is extensive, with a lot of detailed information. For a brief summary, please visit the youth concussion section, under services, on the main page of the website.
In the US, there are 1.6 to 4 million concussions every year. Children are playing competitive sports earlier, and the intensity of sports is increasing at younger ages. Recognition of concussion is becoming more understood among parents and youth coaches, the media is reporting on the problems concussions are causing in professional sports, and diagnosis by pediatricians has also improved. In addition, Colorado law now requires all youth coaches to undergo concussion training, and all children who exhibit symptoms of concussion must be seen by a medical doctor before returning to play.
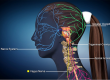
What is concussion? In concussion, MRI and CT scans are typically negative. Those scans are looking for structural problems in the brain such as swelling or bleeding. These problems, if present, result in a more severe brain injury. In cases of concussion, while there are no structural problems, there is a neurologic metabolic energy crisis at the level of the small cells that make up the brain tissue and function. Levels of potassium, sodium, and calcium are increased. This, in addition to other neurochemistry changes in the brain, lead to the injury and concussion symptoms. In most cases, it takes 30 days for the brain chemistry to return to normal levels. During this time, risk of additional brain injury is increased, with subsequent concussions potentially more severe.
Symptoms of Concussion: There are over 21 identified symptoms of concussion. The most common include headache, dizziness, blurred vision, nausea, decreased memory, fatigue, feeling in a fog, and unsteadiness. The post concussion symptom scale, located in the patient form section, lists all 21 symptoms. It is said that concussions are like snowflakes; no two are alike. As a result, there is no “one size fits all” treatment approach.
Factors that may indicate prolonged recovery:
Past medical history of migraine, previous concussions, visual problems, ADHD, and anxiety indicate higher risk of more severe symptoms and longer recovery times. Sustaining a second head injury, even very mild, before full recovery are highly indicative of longer recovery and increased severity of symptoms. Research indicates that immediate dizziness after injury is the symptom associated with a seven fold increase in risk for extended recovery. If the following symptoms within 7 days after the injury, prolonged recovery is also indicated: decreased concentration, fogginess, nausea or vomiting, headache, imbalance, or light/sound sensitivity.
Treatment: In the first days following concussion, rest is the most commonly prescribed treatment. Cognitive rest is as important as physical rest. Cognitive rest includes avoiding loud/busy environments, limiting TV/texting/computer use, limiting reading, etc. Physical rest includes avoiding exertion, with only gentle walking considered. Situations where re-injury can occur due to slowed reflexes and response times such as driving, being at heights, sports practice, recess, and PE are usually avoided initially. The pediatrician, neurologist, or other MD specializing in concussion is the provider who typically guides the gradual return to activity. Most kids with mild concussion recover quickly. Seven to ten days is the most common time for resolution of symptoms in mild concussion, with 80% recovered in three weeks. For those who don’t completely recover in 2-3 weeks, PT is recommended. Earlier intervention, as soon as 1-2 days after injury, is also appropriate in cases of neck pain, headache, and when guidance on proper exercise and activity is desired.
Physical Therapy: In patients with dizziness, neck pain, blurred vision, and/or headache, those treated with specialized vestibular(dizziness) and cervical(neck) PT recover much quicker. In a recent study, 73% of those treated were cleared to return to sport in 8 weeks, compared to 7% of those who were not treated. In PT specialized for concussion, there are six categories we consider.
Vestibular: the vestibular system is our balance and motion sensor. It is responsible for orientation to the environment, balance reactions, eye-head coordination, and acts as a gyroscope for our head. When it is working properly, there is no sensation associated with it. When it is injured, symptoms include disorientation, dizziness, vertigo, motion sickness, blurred vision, and anxiety. Symptoms increase with head or eye motion, being in busy places or in the dark, or when performing visual tasks such as reading or computer work. A detailed assessment of vestibular function in performed.
Oculomotor: Vision is complex. Normal movement and coordination of the eyes result in good binocular vision, depth perception, and clarity. When problems exist in this area, headache at the forehead or behind the eyes can occur, vision can be blurred or strained, and changing focus from far to near or vice versa can be difficult. Testing is completed in this area, and if severe problems are found, a referral to a specialized optometrist may be recommended.
Neck: Whiplash is commonly an additional injury in concussion, due to the forces exerted on the neck and head. This can result in neck pain, neck stiffness, and headache. Pain into the upper back and shoulders can also occur. In addition, injury to the vestibular system can create neck tension and stiffness. Careful examination is done to determine the source of the neck problems.
Headache: Neck problems, visual problems, and vestibular problems can all result in headache. During our assessment, we can determine the contributing factors, with treatments being highly effective. Migraine headaches can also occur as a result of a concussion. Medication may need to be prescribe by the Doctor if this is the case.
Mood: Anxiety is common with injury to the vestibular system. Depression or sadness can also occur when kids are removed from their peers and social settings, or are unable to participate in sports, recess, PE, and social events. Recognizing this and supporting the child and family are important aides to recovery.
Other: Dysautonomia can occur after concussion, leading to irregularities in the modulation of blood pressure and heart rate. This can cause light-headedness or fainting when standing up from lying or sitting, or when standing still for long periods of time. Nutrition and hydration are critical to recovery, and can be addressed during the sessions. Adequate sleep and rest breaks are important for optimal healing and energy. Another challenge that can occur is from social problems, family dynamic issues, or learning disabilities that were present before the concussion. At times, children and their families can cope with these problems on their own, but once a concussion occurs, the coping mechanisms may no longer be effective under the physical and emotional stressors of the injury. Counseling may be recommended if these problems become severe, or are hindering the recovery.
Most PT sessions at NeuroBalance Physical Therapy are 1-2 times per week. Kids can respond very quickly to the therapy, with significant progress occurring in just a few sessions. See the concussion youth section on the services page for more information about this.
Return to Learn: The State of Colorado was the first in the country to enact legislation for return to play in concussions of childhood. One of our local psychologists, Karen McAvoy, was closely involved in this process. She also co authored an article published in Pediatrics, the Journal of the American Academy of Pediatrics titled “Returning to Learning Following a Concussion” in 2013. The following information is a summary of that article, and is common practice in the Denver Area.
The school environment commonly increases symptoms of concussion. Challenges due to cognitive difficulties with academics, along with the overstimulation from the environment such as bright lights, noisy and crowded hallways/lunchrooms/common areas, and visual demands on the focusing system are difficult to tolerate. School adjustments may need to be considered, within the first three weeks when symptoms are greatest. After this time frame, most symptoms in school are gone. Cognitive activity and integration into the stimulating school environment should be coordinated with one lead person at the school (teacher or counselor or nurse) and one member of the medical team. Parents typically start this process, relaying the concerns back and forth from student and school to physician.
Examples of adjustments include:
Periods of physical and cognitive rest during the school day, in a quiet, low lit room.
Early class period dismissal to allow time to move through the hallways, avoiding the crowd of kids.
Reduced exposure to smart boards, computer/video.
Allowing visor/sunglasses in bright spaces.
Lunch in a quiet area with a friend. Earplugs in loud places.
Reduction of repetitive practice assignments.
Assistance for note-taking.
Testing in quiet space with a proctor to decrease distractions.
In more severe or prolonged cases, a formal 504 plan or IEP plan may be written to allow more extensive or lasting adaptations.
The goal of school participation during recovery is to avoid overexerting the brain to the point of aggravating the symptoms. Physical activity during recess and PE is often limited for protection, to reduce the risk of sustaining another concussion. Walking is encouraged, and can be completed in the hallways during PE.
Students should be back to full academic performance and participation before returning to sports or extra curricular activity.
Return to Play: very specific pathways are published in the Return to Play protocol. A link is located at the end of the article. The individual portion of the protocol is usually started along with the return to learn, guided by the Physical Therapist or AT. Julie has extensive experience in all areas of concussion specialized PT, Return to Play protocols, and Return to Learn concepts.
References:
Vestibular Rehabilitation for Dizziness and Balance Disorders after Concussion. Journal of Neurologic Physical Therapy, Vol 34, June 2010.
Cervicovestibular rehabilitation in sport related concussion; a randomized controlled trial. Br J Sports Med, 2014;0:1-6
A Comprehensive Targeted Approach to the Clinical Care of Athletes following Sport Related Concussion. Knee Surg Sports, 2014. 22: 235-246.
Return to Play protocol, along with other excellent information can be found in
“REAP” from the Rocky Mountain Hospital for Children Center for Concussion at this link: http://issuu.com/healthone/docs/reap_oct21